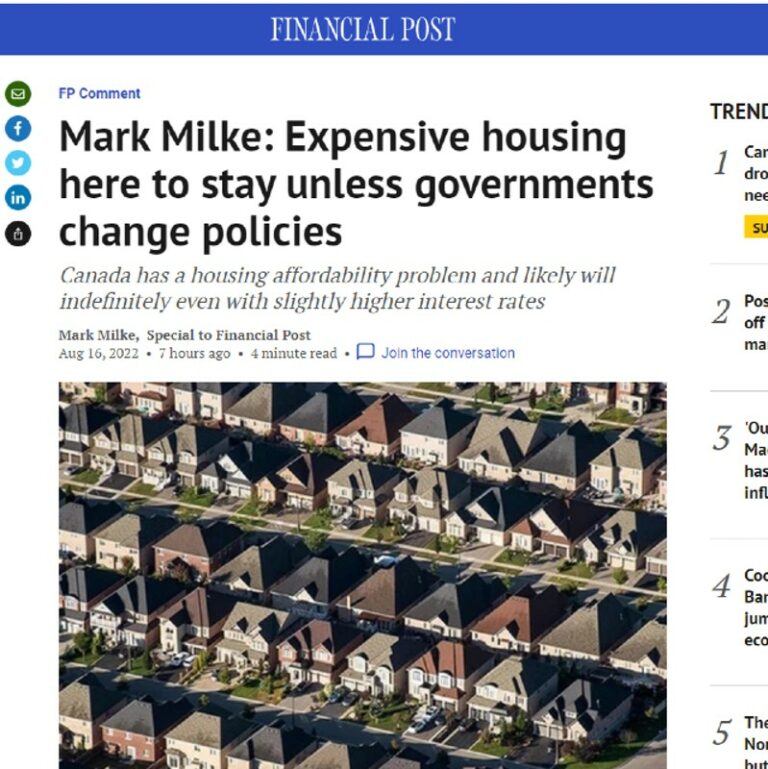
The recent rise in interest rates has dampened demand for home sales in Canada — the hike was inevitable given how historically low rates have been, and that has taken some of the froth off housing prices. However, given how high home prices still are in Canada, a useful question to ask is what can governments do to reverse previous poor policy and permanently increase supply, which has been part of the core problem.
Recent price declines in some markets seem significant. Composite prices in greater Toronto have already dropped by 13 per cent since March and prices in Vancouver are down by 4.5 per cent. However, before millennials or anyone else in the market for a detached home, townhouse or condominium get too excited about a deal, consider that the composite price in Metro Vancouver is still over $1.2 million, while in Toronto it remains over $1.1 million. Those are far from bargain prices.
Those figures did not arrive at such elevated heights overnight. The long-term trend has been heading to unaffordable prices for decades. Demographia International has calculated the rise in Canadian housing costs back to the 1980s by dividing the median house price by gross median household income. It has then tagged the resulting number as affordable (3.0 and under); moderately unaffordable (3.1 to 4.0); seriously unaffordable (4.1 to 5.0); and severely unaffordable (5.1 and above).
To grasp just how expensive Canada has become for housing, in 1987 the house-price-to-income ratio for the entire country was just 3.0, i.e., affordable. By 2020, the median market score for Canada as a whole was double that, or 6.0 — severely unaffordable. Some markets, such as Vancouver and Toronto, are in the double digits of “severely unaffordable” when median prices are compared with incomes.
It’s clear that Canada has a housing affordability problem and likely will indefinitely even with slightly higher interest rates — that is, unless governments begin to address their own roles in making and keeping housing prices high.
On the demand side, immigration levels also contribute to higher prices, but that deserves a full analysis on its own given that the “right” immigration levels address labour supply needs and other issues. Thus, in a report for SecondStreet.org I looked at just the supply side of the problem, as provincial and local governments across the country and across the ideological spectrum could take action without waiting for measures from the federal government.
The problem of constrained supply is severe. As Scotiabank noted last year, Canada needs 1.8 million housing units to reach a balanced market. Now consider how government policy is preventing such a balance and moderate prices.
The first problem on the supply side is regulation and bureaucracy, including how quickly housing developments are approved, while the second factor is escalating fees and taxes.
For example, in 2020, the Canadian Home Builders Association (CHBA) noted that development approvals in Canada take an average of 1.5 to two years to obtain (and more in some cases) — an average of over 20 months for multiple applications, and an average of nearly 12 months for single applications.
As the CHBA also noted, for multiple-unit buildings, for every extra month the builder waits for approval, the average extra monthly cost is $351,500 for a low-rise project and $216,300 for a high-rise project.
Beyond the industry analysis, British Columbia’s NDP government’s 2021 report on housing, chaired by former party leader Joy MacPhail, also noted that there was indeed a problem with regulation and delays. The report urged governments to “clarify and speed up approval processes for the planning and construction of homes,” noting that, “The time needed to steer new housing projects from concept through to ground-breaking can take years” and that this delay “can cost tens of thousands of dollars per new unit …”
The other issue making housing pricier than it ought to be is taxes and fees. The B.C. report found that “some of these fees — notably community amenity contributions — can be unpredictable or inconsistent, causing significant uncertainty, raising costs and compromising supply.”
For its part, the federal government could raise the maximum allowable price for a GST rebate on a new home to $750,000 from the current $450,000, and provide a full rebate of the tax rather than a partial one. That policy change, in combination with the “tens of thousands” of dollars that the MacPhail report said could be saved by speedier approvals, would start to make housing at least slightly more affordable in Canada.
There’s no perfect, magic-bullet remedy to high housing prices, but reduced taxes and fees, plus long-term increased supply as a result of speedier approvals, would contribute to moderating prices.
Mark Milke is the Executive Director of the Aristotle Foundation for Public Policy. He authored the policy brief How to Make Housing Affordable in Canada for SecondStreet.org.
This column was published by the Financial Post on August 16, 2022.
Share on Facebook
Share on Twitter
You can help us continue to research and tell stories about this issue by making a donation or sharing this content with your friends. Be sure to sign up for our updates too!