Share on twitter
Share on facebook
Share on linkedin
Share on email
Play Video
Consider this simple, “bite-sized” illustration involving two pieces of bread.
John Montague was the 4th Earl of Sandwich. He was a statesman and notorious gambler who, during a 24-hour gambling streak in 1762, instructed a cook to prepare his food in such a way that it would not interfere with his game. The cook presented him with a piece of meat between two pieces of bread — no utensils required and could be eaten with one hand while the other hand was free to continue the game!
Now for reasons I don’t fully understand it’s a safe bet that for the rest of your life you will remember – mostly — how the sandwich came to be.
Did etching that into your mind require some secret memory tonic? No. Rather it required something far simpler yet far more powerful: It required telling a story.
For the past thirty years – most of it with the Canadian Taxpayers Federation (CTF) – I’ve been working in the advocacy and public policy field mostly tossing around a lot of big numbers and economic jargon but also, importantly, telling a few stories along the way.
My observation has been that storytelling – or at minimum great narratives – lie at the heart of persuasive and lasting communication. And it’s not just public policy. It’s equally true in arts, business, politics or virtually any walk of life for that matter. Stories stick. Stories capture. Stories move hearts and imaginations in ways numbers cannot.
It’s not that economic data and statistics aren’t vitally important, they are, but that we often look past what’s behind those numbers. We look past what the experiences are of the individuals, families and entrepreneurs that make up economic statistics.
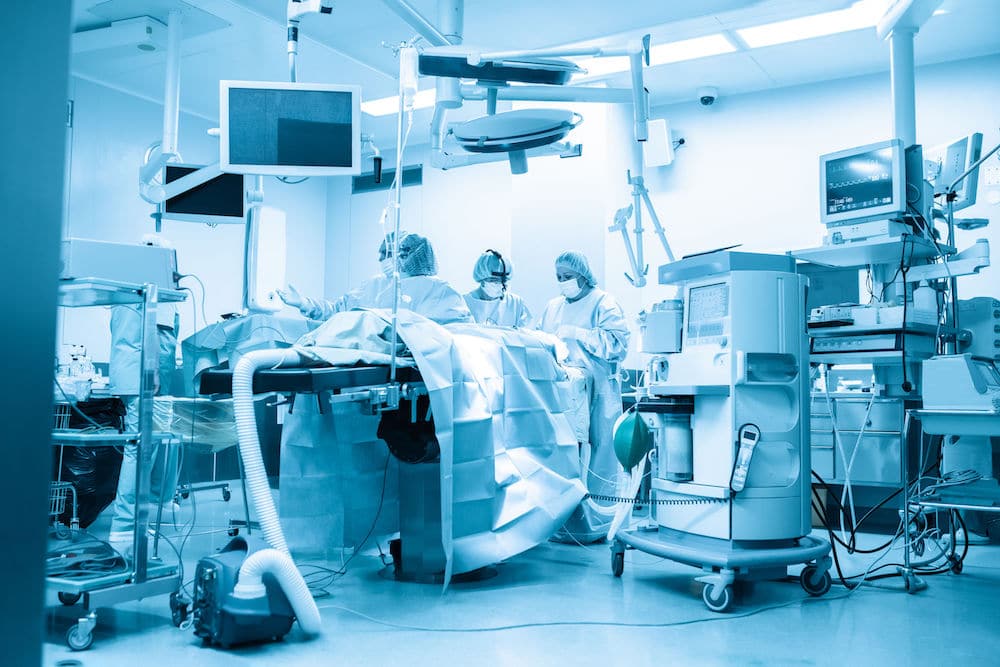
Take hospital waitlists for example. There’s lots of data on the number and length of time people wait, but how often are the stories of people on those waitlists told?
This became a frequent conversation with my friend and former colleague at the CTF Mark Milke (who has also worked with the Fraser Institute and other think tanks) that led us to cobble together a business plan for a new organization. SecondStreet.org would be dedicated to policy research but presented through the experiences and stories of the people affected by public policies.
Almost two-and-a-half years later I’m thrilled to see our vision come to life. To our board and our donors who got behind this vision and made it possible … thank-you!
Of course, this is only a beginning. The willingness of Canadians from coast-to-coast to share their stories will be key for our success going forward. They may not all be as entertaining as John Montague’s gambling-inspired invention of 250 years ago, but they will hopefully stick in hearts and minds and importantly, bring life to the research SecondStreet.org will undertake.
So, if you have an interesting story to share about how government policies have affected your life – in a positive way or a negative way – please send me troy@secondstreet.org or our president, Colin Craig colin@secondstreet.org an e-mail. We’d love to hear from you.
Thanks for visiting our new site!
Troy Lanigan
Founder,
SecondStreet.org
P.S. – If you’re wondering how we chose the name “SecondStreet.org” – give this video a watch – click here
Share on facebook
Share on Facebook
Share on twitter
Share on Twitter
Other Canadians Share Similar Experiences:
Play Video
Don and Jackie, Winnipeg
Play Video
Jerry and Becky, Calgary
Play Video
Troy and Erika, Victoria
Play Video
Jim Jones, Toronto
You can help us continue to research and tell stories about this issue by making a donation
or sharing this content with your friends. Be sure to sign up for our updates too!